52 - 55
- Super User
- Category: Information
- 8276
2022 December;52(4)
Diving Hyperb Med. 2022 December 20;52(4):237–244. doi: 10.28920/dhm52.4.237-244. PMID: 36525681. PMCID: PMC9767826.
Hypoxia signatures in closed-circuit rebreather divers
Daniel Popa1, Craig Kutz2, Morgan Carlile2, Kaighley Brett3, Esteban A Moya4, Frank Powell4, Peter Witucki2, Richard Sadler5, Charlotte Sadler2
1 Hennepin County Medical Center, Department of Emergency Medicine, Division of Hyperbaric and Undersea Medicine, Minneapolis, MN, USA
2 UCSD Department of Emergency Medicine, Division of Hyperbaric and Undersea Medicine, San Diego, CA, USA
3 Canadian Armed Forces, Toronto, Canada
4 UCSD Department of Medicine, Division of Physiology, La Jolla, CA, USA
5 Dive Rescue International, Fort Collins, CO, USA
Corresponding author: Dr Daniel Popa, Hennepin County Medical Center, Department of Emergency Medicine, Division of Hyperbaric and Undersea Medicine, 701 Park Ave, Mail Code P1, Minneapolis, MN 55415, USA
Keywords
Physiology; Rescue; Safety; Technical diving; Training
Abstract
(Popa D, Kutz C, Carlile M, Brett K, Moya EA, Powell F, Witucki P, Sadler R, Sadler C. Hypoxia signatures in closed-circuit rebreather divers. Diving and Hyperbaric Medicine. 2022 December 20;52(4):237–244. doi: 10.28920/dhm52.4.237-244. PMID: 36525681. PMCID: PMC9767826.)
Introduction: Faults or errors during use of closed-circuit rebreathers (CCRs) can cause hypoxia. Military aviators face a similar risk of hypoxia and undergo awareness training to determine their ‘hypoxia signature’, a personalised, reproducible set of symptoms. We aimed to establish a hypoxia signature among divers, and to investigate their ability to detect hypoxia and self-rescue while cognitively overloaded.
Methods: Eight CCR divers and 12 scuba divers underwent an initial unblinded hypoxia exposure followed by three trials; a second hypoxic trial and two normoxic trials in randomised order. Hypoxia was induced by breathing on a CCR with no oxygen supply. Subjects pedalled on a cycle ergometer while playing a neurocognitive computer game to simulate real world task loading. Subjects identified hypoxia symptoms by pointing to a board listing common hypoxia symptoms, and were instructed to perform a ‘bailout’ procedure to mimic self-rescue if they perceived hypoxia. Divers were prompted to bailout if peripheral oxygen saturation fell to 75%, or after six minutes during normoxic trials. Subsequently we interviewed subjects to determine their ability to distinguish hypoxia from normoxia.
Results: Ninety-five percent of subjects (19/20) showed agreement between unblinded and blinded hypoxia symptoms. Subjects correctly identified the gas mixture in 85% of the trials. During unblinded hypoxia, only 25% (5/20) of subjects performed unprompted bailout. Fifty-five percent of subjects (11/20) correctly performed the bailout but only when prompted, while 15% (3/20) were unable to bailout despite prompting. During blinded hypoxia 45% of subjects (9/20) performed the bailout unprompted while 15% (3/20) remained unable to bailout despite prompting.
Conclusions: Although our data support a normobaric hypoxia signature among both CCR and scuba divers under experimental conditions, most subjects were unable to recognise hypoxia in real time and perform a self-rescue unprompted, although this improved in the second hypoxia trial. These results do not support hypoxia exposure training for CCR divers.
Copyright: This article is the copyright of the authors who grant Diving and Hyperbaric Medicine a non-exclusive licence to publish the article in electronic and other forms.
Publication Type: Original article
Full article available here.
2022 December;52(4)
Diving Hyperb Med. 2022 December 20;52(4):245−259. doi: 10.28920/dhm52.4.245-259. PMID: 36525682. PMCID: PMC9767825.
A review of accelerated decompression from heliox saturation in commercial diving emergencies
Jean-Pierre Imbert1, Jean-Yves Massimelli2, Ajit Kulkarni3, Lyubisa Matity4, Philip Bryson5
1 Divetech, 1543 ch. des vignasses, Biot, France
2 Flash Tekk Engineering, Singapore
3 Hyperbaric Solutions, Bandra East, Mumbai, India
4 Hyperbaric and Tissue Viability Unit, Gozo General Hospital, Malta
5 International SOS, Forest Grove House, Aberdeen, UK
Corresponding author: Dr Philip Bryson, International SOS, Forest Grove House, Foresterhill Road, Aberdeen, AB25 2ZP, UK
Keywords
Decompression sickness; Diving incidents; Emergency ascent; Emergency response; Saturation diving
Abstract
(Imbert J-P, Massimelli J-Y, Kulkarni A, Matity L, Bryson P. A review of accelerated decompression from heliox saturation in commercial diving emergencies. Diving and Hyperbaric Medicine. 2022 December 20;52(4):245−259. doi: 10.28920/dhm52.4.245-259. PMID: 36525682. PMCID: PMC9767825.)
Introduction: Saturation diving is a specialised method of intervention in offshore commercial diving. Emergencies may require the crew to be evacuated from the diving support vessel. Because saturation divers generally need several days to reach surface, the emergency evacuation of divers is based on dedicated hyperbaric rescue systems. There are still potential situations for which these systems cannot be used or deployed, and where an emergency decompression provides an alternative solution.
Methods: Our objective was to describe historical cases and assess the benefit of emergency decompressions, with the collection of data from the authors’ direct experience and networks, providing witness or first-hand information.
Results: We documented three cases of emergency decompression following bell evacuations, and six cases of accelerated decompression performed in the chamber or hyperbaric rescue chamber. Review of these cases showed: 1) the complicated nature of such emergencies that make decisions difficult; 2) the variety of solutions implemented; and 3) the surprisingly safe and successful outcomes of several operations. Analysis of the accelerated decompression occurrences allowed derivation of the options used; upward initial excursion, increased chamber partial pressure of oxygen associated to increased ascent rates, and inert gas switching. We identified four published procedures for accelerated decompression.
Conclusions: Despite modern hyperbaric rescue systems, accelerated decompression remains an essential tool in case of emergency. The diving industry needs clear guidance on what can be achieved, depending on the saturation depth and the level of emergency.
Copyright: This article is the copyright of the authors who grant Diving and Hyperbaric Medicine a non-exclusive licence to publish the article in electronic and other forms.
Publication Type: Original article
Full article available here.
2022 December;52(4)
Diving Hyperb Med. 2022 December 20;52(4):260−270. doi: 10.28920/dhm52.4.260-270. PMID: 36525683. PMCID: PMC10017198.
Effects of high oxygen tension on healthy volunteer microcirculation
Nicolas Cousin1, Julien Goutay1, Patrick Girardie1, Raphaël Favory1, Elodie Drumez2, Daniel Mathieu1, Julien Poissy1, Erika Parmentier1, Thibault Duburcq1
1 Pôle de réanimation, hôpital Roger Salengro, CHU Lille, Lille, France
2 Unité de méthodologie – biostatistique et data management, CHU Lille, Lille, France
Corresponding author: Dr Thibault Duburcq, Centre Hospitalier Universitaire de Lille, Hôpital Roger Salengro – Centre de réanimation, Avenue du Professeur Emile Laine , 59037 LILLE Cedex, France
Keywords
Hyperbaric oxygen treatment; Hyperoxia; Laser Doppler flowmetry; Near-infrared spectroscopy; Perfusion
Abstract
(Cousin N, Goutay J, Girardie P, Favory R, Drumez E, Mathieu D, Poissy J, Parmentier E, Duburcq. Effects of high oxygen tension on healthy volunteer microcirculation. Diving and Hyperbaric Medicine. 2022 December 20;52(4):260−270. doi: 10.28920/dhm52.4.260-270. PMID: 36525683. PMCID: PMC10017198.)
Introduction: Previous studies have highlighted hyperoxia-induced microcirculation modifications, but few have focused on hyperbaric oxygen (HBO) effects. Our primary objective was to explore hyperbaric hyperoxia effects on the microcirculation of healthy volunteers and investigate whether these modifications are adaptative or not.
Methods: This single centre, open-label study included 15 healthy volunteers. Measurements were performed under five conditions: T0) baseline value (normobaric normoxia); T1) hyperbaric normoxia; T2) hyperbaric hyperoxia; T3) normobaric hyperoxia; T4) return to normobaric normoxia. Microcirculatory data were gathered via laser Doppler, near-infrared spectroscopy and transcutaneous oximetry (PtcO2). Vascular-occlusion tests were performed at each step. We used transthoracic echocardiography and standard monitoring for haemodynamic investigation.
Results: Maximal alterations were observed under hyperbaric hyperoxia which led, in comparison with baseline, to arterial hypertension (mean arterial pressure 105 (SD 12) mmHg vs 95 (11), P < 0.001) and bradycardia (55 (7) beats·min-1 vs 66 (8), P < 0.001) while cardiac output remained unchanged. Hyperbaric hyperoxia also led to microcirculatory vasoconstriction (rest flow 63 (74) vs 143 (73) perfusion units, P < 0.05) in response to increased PtcO2 (104.0 (45.9) kPa vs 6.3 (2.4), P < 0.0001); and a decrease in laser Doppler parameters indicating vascular reserve (peak flow 125 (89) vs 233 (79) perfusion units, P < 0.05). Microvascular reactivity was preserved in every condition.
Conclusions: Hyperoxia significantly modifies healthy volunteer microcirculation especially during HBO exposure. The rise in PtcO2 promotes an adaptative vasoconstrictive response to protect cellular integrity. Microvascular reactivity remains unaltered and vascular reserve is mobilised in proportion to the extent of the ischaemic stimulus.
Copyright: This article is the copyright of the authors who grant Diving and Hyperbaric Medicine a non-exclusive licence to publish the article in electronic and other forms.
Publication Type: Original article
Full article available here.
2022 December;52(4)
Diving Hyperb Med. 2022 December 20;52(4):271−276. doi: 10.28920/dhm52.4.271-276. PMID: 36525684. PMCID: PMC10026386.
Delayed treatment for decompression illness: factors associated with long treatment delays and treatment outcome
Sofia A Sokolowski1, Anne K Räisänen-Sokolowski2,3, Laura J Tuominen2,4, Richard V Lundell2,5
1 University of Eastern Finland, Kuopio, Finland
2 Department of Pathology, Helsinki University, Helsinki, Finland
3 HUSLAB, Pathology, Helsinki University Hospital, Helsinki, Finland
4 Department of Anaesthesia, Tampere University Hospital, Tampere, Finland
5 Diving Medical Centre, Centre for Military Medicine, Finnish Defence Forces, Helsinki, Finland
Corresponding author: Dr Richard V Lundell, Diving Medical Centre, Centre for Military Medicine, Finnish Defence Forces, Helsinki, Finland
Keywords
Decompression sickness; Hyperbaric oxygen treatment; Epidemiology; First aid oxygen; Remote locations; Treatment sequelae
Abstract
(Sokolowski SA, Räisänen-Sokolowski AK, Tuominen LJ, Lundell RV. Delayed treatment for decompression illness: factors associated with long treatment delays and treatment outcome. Diving and Hyperbaric Medicine. 2022 December 20;52(4):271−276. doi: 10.28920/dhm52.4.271-276. PMID: 36525684. PMCID: PMC10026386.)
Introduction: Effectiveness of delayed hyperbaric oxygen treatment (HBOT) for decompression illness (DCI) and factors affecting treatment delays have not been studied in large groups of patients.
Methods: This retrospective study included 546 DCI patients treated in Finland in the years 1999–2018 and investigated factors associated with recompression delay and outcome. Treatment outcome was defined as fully recovered or presence of residual symptoms on completion of HBOT. The symptoms, use of first aid oxygen, number of recompression treatments needed and characteristics of the study cohort were also addressed.
Results: Delayed HBOT (> 48 h) remained effective with final outcomes similar to those treated within 48 h. Cardio-pulmonary symptoms were associated with a shorter treatment delay (median 15 h vs 28 h without cardiopulmonary symptoms, P < 0.001), whereas mild sensory symptoms were associated with a longer delay (48 vs 24 h, P < 0.001). A shorter delay was also associated with only one required HBOT treatment (median 24 h vs 34 h for those requiring multiple recompressions) (P = 0.002). Tinnitus and hearing impairment were associated with a higher proportion of incomplete recoveries (78 and 73% respectively, P < 0.001), whereas a smaller proportion of cases with tingling/itching (15%, P = 0.03), nausea (27%, P = 0.03), motor weakness (33%, P = 0.05) and visual disturbances (36%, P = 0.04) exhibited residual symptoms. Patients with severe symptoms had a significantly shorter delay than those with mild symptoms (median 24 h vs 36 h respectively, P < 0.001), and a lower incidence of complete recovery.
Conclusions: Delayed HBOT remains an effective and useful intervention. A shorter delay to recompression is associated with fewer recompressions required to achieve recovery or recovery plateau.
Copyright: This article is the copyright of the authors who grant Diving and Hyperbaric Medicine a non-exclusive licence to publish the article in electronic and other forms.
Publication Type: Original article
Full article available here.
2022 December;52(4)
Diving Hyperb Med. 2022 December 20;52(4):277−280. doi: 10.28920/dhm52.4.277-280. PMID: 36525685. PMCID: PMC10017199.
Descriptive study of decompression illness in a hyperbaric medicine centre in Bangkok, Thailand from 2015 to 2021
Pitchaya Chevasutho1, Hansa Premmaneesakul2, Atipong Sujiratana2
1 Occupational Medicine Center, Chonburi Hospital, Chonburi, Thailand
2 Maritime Medicine Division, Somdech Phra Pinklao Hospital, Naval Medical Department, Bangkok, Thailand
Corresponding author: Dr Pitchaya Chevasutho, Occupational Medicine Center, Chonburi Hospital, 69 Moo 2, Sukhumvit Rd, Chonburi, Thailand 20000
Keywords
Arterial gas embolism; Decompression sickness; Diving incidents; Hyperbaric oxygen treatment
Abstract
(Chevasutho P, Premmaneesakul H, Sujiratana A. Descriptive study of decompression illness in a hyperbaric medicine centre in Bangkok, Thailand from 2015 to 2021. Diving and Hyperbaric Medicine. 2022 December 20;52(4):277−280. doi: 10.28920/dhm52.4.277-280. PMID: 36525685. PMCID: PMC10017199.)
Introduction: This study aimed to determine the characteristics of decompression illness patients and their treatment outcomes, at the Center of Hyperbaric Medicine, Somdech Phra Pinklao Hospital, one of the largest centres in Thailand.
Methods: Past medical records of patients with decompression illness from 2015 to 2021 were retrieved and analysed.
Results: Ninety-eight records of diving-related illness from 97 divers were reviewed. Most of the divers were male (n = 50), Thai (n = 86), and were certified at least open water or equivalent (n = 88). On-site first aid oxygen inhalation was provided to 17 divers. Decompression sickness (DCS) cases were characterised according to organ systems involved. The most prominent organ system involved was neurological (57%), followed by mixed organs (28%), musculoskeletal (13%), and pulmonary (2%). There were three cases of arterial gas embolism (AGE). Median presentation delay was three days. Ninety patients were treated with US Navy Treatment Table 6. At the end of their hyperbaric oxygen treatment, most divers (65%) recovered completely.
Conclusions: Despite oxygen first aid being given infrequently and long delays before definitive treatment, treatment outcome was satisfactory. Basic knowledge and awareness of diving-related illnesses should be promoted among divers and related personnel in Thailand along with further studies.
Copyright: This article is the copyright of the authors who grant Diving and Hyperbaric Medicine a non-exclusive licence to publish the article in electronic and other forms.
Publication Type: Original article
Full article available here.
2022 December;52(4)
Diving Hyperb Med. 2022 December 20;52(4):281−285. doi: 10.28920/dhm52.4.281-285. PMID: 36525686. PMCID: PMC10017197.
Agreement between ultrasonic bubble grades using a handheld self-positioning Doppler product and 2D cardiac ultrasound
Oscar Plogmark1,2, Carl Hjelte1,2,3, Magnus Ekström1, Oskar Frånberg2,4
1 Lund University, Faculty of Medicine, Department of Clinical Sciences Lund, Respiratory Medicine and Allergology, Lund, Sweden
2 Swedish Armed Forces Diving and Naval Medicine Center, Swedish Armed Forces, Karlskrona, Sweden
3 Sahlgrenska University Hospital, Anesthesia and Intensive Care. Gothenburg, Sweden
4 Blekinge Institute of Technology, Department of Mathematics and Natural Science, Karlskrona, Sweden
Corresponding author: Oscar Plogmark, Sten Bergmans väg 21, 121 46 Johanneshov, Sweden
Keywords
Decompression; Decompression illness; Decompression sickness; Diving research; Echocardiography; Ultrasound; Venous gas emboli
Abstract
(Plogmark O, Hjelte C, Ekström M, Frånberg O. Agreement between ultrasonic bubble grades using a handheld self-positioning Doppler product and 2D cardiac ultrasound. Diving and Hyperbaric Medicine. 2022 December 20;52(4):281−285. doi: 10.28920/dhm52.4.281-285. PMID: 36525686. PMCID: PMC10017197.)
Introduction: Intravascular bubble load after decompression can be detected and scored using ultrasound techniques that measure venous gas emboli (VGE). The aim of this study was to analyse the agreement between ultrasonic bubble grades from a handheld self-positioning product, the O’DiveTM, and cardiac 2D ultrasound after decompression.
Methods: VGE were graded with both bilateral subclavian vein Doppler ultrasound (modified Spencer scale) and 2D cardiac images (Eftedal Brubakk scale). Agreement was analysed using weighted kappa (Kw). Analysis with Kw was made for all paired grades, including measurements with and without zero grades, and for each method’s highest grades after each dive.
Results: A total of 152 dives yielded 1,113 paired measurements. The Kw agreement between ultrasound VGE grades produced by cardiac 2D images and those from the O’Dive was ‘fair’; when zero grades were excluded the agreement was ‘poor’. The O’Dive was found to have a lower sensitivity to detect VGE compared to 2D cardiac image scoring.
Conclusions: Compared to 2D cardiac image ultrasound, the O’Dive yielded generally lower VGE grades, which resulted in a low level of agreement (fair to poor) with Kw.
Copyright: This article is the copyright of the authors who grant Diving and Hyperbaric Medicine a non-exclusive licence to publish the article in electronic and other forms.
Publication Type: Original article
Full article available here.
2022 December;52(4)
Diving Hyperb Med. 2022 December 20;52(4):286−288. doi: 10.28920/dhm52.4.286-288. PMID: 36525687. PMCID: PMC10017196.
Electric shock leading to acute lung injury in a scuba diver
Kelly Johnson-Arbor
Department of Plastic and Reconstructive Surgery, MedStar Georgetown University Hospital, Washington DC, USA
Corresponding author: Dr Kelly Johnson-Arbor, Department of Plastic and Reconstructive Surgery, MedStar Georgetown University Hospital, 3800 Reservoir Road NW, Washington DC, 20007, USA
Keywords
Burns; Diving; Electric injuries; Salt water aspiration
Abstract
(Johnson-Arbor K. Electric shock leading to acute lung injury in a scuba diver. Diving and Hyperbaric Medicine. 2022 December 20;52(4):286−288. doi: 10.28920/dhm52.4.286-288. PMID: 36525687. PMCID: PMC10017196.)
Introduction: Electrical injuries are a rarely reported complication of scuba diving.
Case report: A 33-year-old woman wore a 12-volt heated shirt designed for motorcycling, powered by a canister light battery, while scuba diving. A leak in her drysuit allowed water to make contact with an electrified connector from the heated shirt, and she experienced painful electrical shocks. She was able to disconnect the power source and finish the dive, but she developed progressive fevers and dyspnoea several hours later. She was diagnosed with acute lung injury and treated with bronchodilators. Her symptoms resolved over subsequent weeks.
Discussion: Acute lung injury is rarely reported after low voltage electrical injury. In this case, the use of a heated shirt that was not intended for underwater activities heightened the patient’s risk for electric shock that likely resulted in aspiration of sea water and subsequent acute lung injury. To reduce risk of injury, divers should use equipment that is designed for underwater submersion. Medical professionals who treat the diving population should be aware that divers may use modified equipment that increases the risk of diving-related complications.
Copyright: This article is the copyright of the authors who grant Diving and Hyperbaric Medicine a non-exclusive licence to publish the article in electronic and other forms.
Publication Type: Original article
Full article available here.
- Super User
- Category: Information
- 8355
2023 March;53(1)
Diving Hyperb Med. 2023 March 31;53(1):2−6. doi: 10.28920/dhm53.1.2-6. PMID: 36966516. PMCID: PMC10318177.
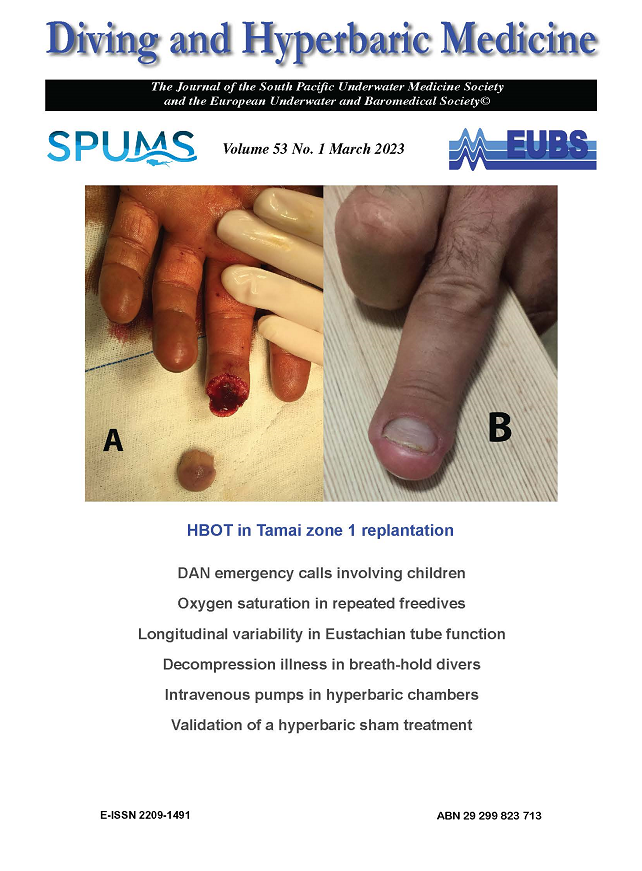
Effects of external bleeding and hyperbaric oxygen treatment on Tamai zone 1 replantation
Yavuz Tuluy1, Alper Aksoy2, Emin Sır3
1 Department of Plastic Reconstructive and Aesthetic Surgery, Turgutlu State Hospital, Manisa, Turkey
2 Konur Hospital, Department of Plastic Reconstructive and Aesthetic Surgery, Bursa, Turkey
3 İzmir Kavram Vocational School, Department of Plastic Reconstructive and Aesthetic Surgery, İzmir, Turkey
Corresponding author: Dr Yavuz Tuluy, Plastic, Reconstructive and Aesthetic Surgery, Manisa Turgutlu State Hospital, Turgutlu, Manisa, 45000, Turkey
Keywords
Finger; Microsurgery; Reperfusion; Surgery
Abstract
(Tuluy Y, Aksoy A, Sir E. Effects of external bleeding and hyperbaric oxygen treatment on Tamai zone 1 replantation. Diving and Hyperbaric Medicine. 2023 March 31;53(1):2−6. doi: 10.28920/dhm53.1.2-6. PMID: 36966516. PMCID: PMC10318177.)
Introduction: Tamai zone 1 replantation poses a challenge due to the very small size of the vascular structures; often there is no vein for anastomosis. Replantation may have to be done with only an arterial anastomosis. In our study, we aimed to evaluate the success of replantation by combining external bleeding and hyperbaric oxygen treatment (HBOT) in Tamai zone 1 replantation.
Methods: Between January 2017 and October 2021, 17 finger replantation patients who underwent artery-only anastomosis due to Tamai zone 1 amputation received 20 sessions of HBOT with external bleeding after the 24th postoperative hour. Finger viability was assessed at the end of treatment. A retrospective review of outcomes was performed.
Results: Seventeen clean-cut finger amputation patients were operated on under digital block anesthesia with a finger tourniquet. No blood transfusion was required. In one patient, complete necrosis developed and stump closure was performed. Partial necrosis was observed in three patients and healed secondarily. Replantation in the remaining patients was successful.
Conclusions: Vein anastomosis is not always possible in fingertip replantation. In Tamai zone 1 replantation with artery-only anastomosis, post-operative HBOT with induced external bleeding appeared to shorten the hospital stay and was associated with a high proportion of successful outcomes.
Copyright: This article is the copyright of the authors who grant Diving and Hyperbaric Medicine a non-exclusive licence to publish the article in electronic and other forms.
Publication Type: Original article
Full article available here.
Diving Hyperb Med. 2023 March 31;53(1):7−15. doi: 10.28920/dhm53.1.7-15. PMID: 36966517. PMCID: PMC10318175.
A review of 149 Divers Alert Network emergency call records involving diving minors
Elizabeth T Helfrich1, Camilo M Saraiva1, James M Chimiak1, Matias Nochetto1
1 Divers Alert Network, Durham (NC), USA
Corresponding author: Dr Matias Nochetto, Vice President, Medical Services, Divers Alert Network, Durham NC, USA
Keywords
Arterial gas embolism; Children; Decompression illness; Pulmonary barotrauma; Scuba diving
Abstract
(Helfrich ET, Saraiva CM, Chimiak JM, Nochetto M. A review of 149 Divers Alert Network emergency call records involving diving minors. Diving and Hyperbaric Medicine. 2023 March 31;53(1):7−15. doi: 10.28920/dhm53.1.7-15. PMID: 36966517. PMCID: PMC10318175.)
Introduction: Minors have been scuba diving for decades, and while the initial concerns about potential long-term complications related to bone development appear to be unfounded, the incidence of scuba diving injuries among them has been poorly studied.
Methods: We reviewed 10,159 cases recorded in the DAN Medical Services call center database from 2014 through 2016 and identified 149 cases of injured divers younger than 18 years. Records were analysed for case categorisation on the most common dive injuries. Information about demographics, level of training, risk factors, and relevant behavioural aspects were collected when available.
Results: While the most common reason for the call was to rule out decompression sickness, the majority of cases pertained to ear and sinus issues. However, 15% of the dive-related injuries involving minors had a final diagnosis of pulmonary barotrauma (PBt). While no reliable data is available on the incidence of PBt in adult divers, the authors’ impression based on personal experience suggests that the number of cases of PBt in minors trends higher than in the general diving population. The narratives on some relevant records describe unmanageable levels of anxiety leading to panic.
Conclusions: Based on the results and narratives on these cases, it is reasonable to infer that psychological immaturity, suboptimal management of adverse situations, and inadequate supervision might have led to severe injuries among these minor divers.
Copyright: This article is the copyright of the authors who grant Diving and Hyperbaric Medicine a non-exclusive licence to publish the article in electronic and other forms.
Publication Type: Original article
Full article available here.
Diving Hyperb Med. 2023 March 31;53(1):16–23. doi: 10.28920/dhm53.1.16-23. PMID: 36966518. PMCID: PMC10318178.
Underwater pulse oximetry reveals increased rate of arterial oxygen desaturation across repeated freedives to 11 metres of freshwater
Eric Mulder1, Arne Sieber1,2, Chris McKnight3, Erika Schagatay1,4
1 Environmental Physiology Group, Department of Health Sciences, Mid Sweden University, Östersund, Sweden
2 OXYGEN Scientific GmbH, Feldkirchen, Austria
3 Sea Mammal Research Unit, Scottish Oceans Institute, University of St Andrews, St Andrews, Scotland
4 Swedish Winter Sports Research Centre, Mid Sweden University, Östersund, Sweden
Corresponding author: Eric Mulder, Mid Sweden University, Kunskapens väg 8, 83125 Östersund, Sweden
Keywords
Breath-hold diving; Diving reflex; Hypoxia; Oxygen consumption; Safety; Unconsciousness
Abstract
(Mulder E, Sieber A, McKnight C, Shagatay E. Underwater pulse oximetry reveals increased rate of arterial oxygen desaturation across repeated freedives to 11 metres of freshwater. Diving and Hyperbaric Medicine. 2023 March 31;53(1):16−23. doi: 10.28920/dhm53.1.16-23. PMID: 36966518. PMCID: PMC10318178.)
Introduction: Recreational freedivers typically perform repeated dives to moderate depths with short recovery intervals. According to freediving standards, these recovery intervals should be twice the dive duration; however, this has yet to be supported by scientific evidence.
Methods: Six recreational freedivers performed three freedives to 11 metres of freshwater (mfw), separated by 2 min 30 s recovery intervals, while an underwater pulse oximeter measured peripheral oxygen saturation (SpO2) and heart rate (HR).
Results: Median dive durations were 54.0 s, 103.0 s and 75.5 s (all dives median 81.5 s). Median baseline HR was 76.0 beats per minute (bpm), which decreased during dives to 48.0 bpm in dive one, 40.5 bpm in dive two and 48.5 bpm in dive three (all P < 0.05 from baseline). Median pre-dive baseline SpO2 was 99.5%. SpO2 remained similar to baseline for the first half of the dives, after which the rate of desaturation increased during the second half of the dives with each subsequent dive. Lowest median SpO2 after dive one was 97.0%, after dive two 83.5% (P < 0.05 from baseline) and after dive three 82.5% (P < 0.01 from baseline). SpO2 had returned to baseline within 20s after all dives.
Conclusions: We speculate that the enhanced rate of arterial oxygen desaturation across the serial dives may be attributed to a remaining ‘oxygen debt’, leading to progressively increased oxygen extraction by desaturated muscles. Despite being twice the dive duration, the recovery period may be too short to allow full recovery and to sustain prolonged serial diving, thus does not guarantee safe diving.
Copyright: This article is the copyright of the authors who grant Diving and Hyperbaric Medicine a non-exclusive licence to publish the article in electronic and other forms.
Publication Type: Original article
Full article available here.
Diving Hyperb Med. 2023 March 31;53(1):24−30. doi: 10.28920/dhm53.1.24-30. PMID: 36966519. PMCID: PMC10325792.
Intraindividual variability of the Eustachian tube function: a longitudinal study in a pressure chamber
Nele Peters1*, Stefanie Jansen1*, Jens P Klußmann1, Moritz F Meyer2
1 Department of Otorhinolaryngology, Head and Neck Surgery, University of Cologne, Cologne, Germany
2 Department of Otorhinolaryngology, Head and Neck Surgery, University Hospital Essen, University Duisburg-Essen, Essen, Germany
* Contributed equally to this work
Corresponding author: Dr Moritz F Meyer, Department of Otorhinolaryngology, Head and Neck Surgery, University Hospital Essen, Hufelandstraße 55, 45147 Essen, Germany
Keywords
Diving; Ear barotrauma; Ears; Middle ear; Pressure equalisation
Abstract
(Peters N, Jansen S, Klußmann JP, Meyer MF. Intraindividual variability of the Eustachian tube function: a longitudinal study in a pressure chamber. Diving and Hyperbaric Medicine. 2023 March 31;53(1):24−30. doi: 10.28920/dhm53.1.24-30. PMID: 36966519. PMCID: PMC10325792.)
Introduction: The Eustachian tube (ET) is essential for fast and direct pressure equalisation between middle ear and ambient pressure. It is not yet known to what extent Eustachian tube function in healthy adults changes in a weekly periodicity due to internal and external factors. This question is particularly interesting with regard to scuba divers among whom there is a need to evaluate intraindividual ET function variability.
Methods: Continuous impedance measurement in a pressure chamber was performed three times at one-week intervals between measurements. Twenty healthy participants (40 ears) were enrolled. Using a monoplace hyperbaric chamber, individual subjects were exposed to a standardised pressure profile consisting of a 20 kPa decompression over 1 min, a 40 kPa compression over 2 min, and a 20 kPa decompression over 1 min. Measurements of Eustachian tube opening pressure (ETOP), opening duration (ETOD), and opening frequency (ETOF) were made. Intraindividual variability was assessed.
Results: Mean ETOD during compression (actively induced pressure equalisation) on the right side was 273.8 (SD 158.8) ms, 259.4 (157.7) ms, and 249.2 (154.1) (Chi-square 7.30, P = 0.026) across weeks 1−3. Mean ETOD for both sides was 265.6 (153.3) ms, 256.1 (154.6) ms, and 245.7 (147.8) (Chi-square10.00, P = 0.007) across weeks 1−3. There were no other significant differences in ETOD, ETOP and ETOF across the three weekly measurements.
Conclusions: This longitudinal study suggests low week-to-week intraindividual variability of Eustachian tube function.
Copyright: This article is the copyright of the authors who grant Diving and Hyperbaric Medicine a non-exclusive licence to publish the article in electronic and other forms.
Publication Type: Original article
Full article available here.
Diving Hyperb Med. 2023 March 31;53(1):31−41. doi: 10.28920/dhm53.1.31-41. PMID: 36966520. PMCID: PMC10106275.
The risk of decompression illness in breath-hold divers: a systematic review
S Lesley Blogg1, Frauke Tillmans2, Peter Lindholm3
1 SLB Consulting, Newbiggin-on-Lune, Cumbria, UK
2 Divers Alert Network, Durham, USA
3 Department of Emergency Medicine, University of California, San Diego, CA, USA
Corresponding author: Professor Peter Lindholm, 200 W Arbor Drive, MC8676, San Diego, CA 92103, USA
Keywords
Arterial gas embolism; Breath-hold diving; Decompression sickness; Diving; Freediving; Snorkelling; Spearfishing
Abstract
(Blogg SL, Tillmans F, Lindholm P. The risk of decompression illness in breath-hold divers: a systematic review. Diving and Hyperbaric Medicine. 2023 March 31;53(1):31−41. doi: 10.28920/dhm53.1.31-41. PMID: 36966520. PMCID: PMC10106275.)
Introduction: Breath-hold (BH) diving has known risks, for example drowning, pulmonary oedema of immersion and barotrauma. There is also the risk of decompression illness (DCI) from decompression sickness (DCS) and/or arterial gas embolism (AGE). The first report on DCS in repetitive freediving was published in 1958 and from then there have been multiple case reports and a few studies but no prior systematic review or meta-analysis.
Methods: We undertook a systematic literature review to identify articles available from PubMed and Google Scholar concerning breath-hold diving and decompression illness up to August 2021.
Results: The present study identified 17 articles (14 case reports, three experimental studies) covering 44 incidences of DCI following BH diving.
Conclusions: This review found that the literature supports both DCS and AGE as potential mechanisms for DCI in BH divers; both should be considered a risk for this cohort of divers, just as for those breathing compressed gas while underwater.
Copyright: This article is the copyright of the authors who grant Diving and Hyperbaric Medicine a non-exclusive licence to publish the article in electronic and other forms.
Publication Type: Review article
Full article available here.
Diving Hyperb Med. 2023 March 31;53(1):42−50. doi: 10.28920/dhm53.1.42-50. PMID: 36966521. PMCID: PMC10318176.
Safety and performance of intravenous pumps and syringe drivers in hyperbaric environments
Aisha Al Balushi1,2, David Smart2
1 National Hyperbaric Medicine Centre, Royal Hospital, Muscat, Sultanate of Oman
2 Department of Diving and Hyperbaric Medicine, Royal Hobart Hospital, Hobart, Tasmania, Australia
Corresponding author: Dr Aisha Al Balushi, Diving and Hyperbaric Medicine Fellow, National Hyperbaric Medicine Centre, Royal Hospital, Ghala St, Muscat, Sultanate of Oman
Keywords
Equipment; Fire risk; Hyperbaric oxygen; Infusion devices; Safety; Risk assessment
Abstract
(Al Balushi A, Smart D. Safety and performance of intravenous pumps and syringe drivers in hyperbaric environments. Diving and Hyperbaric Medicine. 2023 March 31;53(1):42−50. doi: 10.28920/dhm53.1.42-50. PMID: 36966521. PMCID: PMC10318176.)
Introduction: Critically ill patients require continuation of their care when receiving hyperbaric oxygen treatment. This care may be facilitated via portable electrically powered devices such as intravenous (IV) infusion pumps and syringe drivers, which may create risks in the absence of a comprehensive safety evaluation. We reviewed published safety data for IV infusion pumps and powered syringe drivers in hyperbaric environments and compared the evaluation processes to key requirements documented in safety standards and guidelines.
Methods: A systematic literature review was undertaken to identify English language papers published in the last 15 years, describing the safety evaluations of IV pumps and/or syringe drivers for use in hyperbaric environments. Papers were critically assessed in relation to the requirements of international standards and safety recommendations.
Results: Eight studies of IV infusion devices were identified. There were deficiencies in the published safety evaluations of IV pumps for hyperbaric use. Despite a simple, published process for evaluating new devices, and available guidelines for fire safety, only two devices had comprehensive safety assessments. Most studies focused only on whether the device functioned normally under pressure and did not consider implosion/explosion risk, fire safety, toxicity, oxygen compatibility or risk of pressure damage.
Conclusions: Intravenous infusion (and other electrically powered) devices require comprehensive assessment before use under hyperbaric conditions. This would be enhanced by a publicly accessible database hosting the risk assessments. Facilities should conduct their own assessments specific to their environment and practices.
Copyright: This article is the copyright of the authors who grant Diving and Hyperbaric Medicine a non-exclusive licence to publish the article in electronic and other forms.
Publication Type: Review article
Full article available here.
Diving Hyperb Med. 2023 March 31;53(1):51–54. doi: 10.28920/dhm53.1.51-54. PMID: 36966522. PMCID: PMC10318180.
Validation of sham treatment in hyperbaric medicine: a randomised trial
Pierre Louge1, Rodrigue Pignel1, Jacques Serratrice2, Jerome Stirnemann2
1 Diving and hyperbaric Unit, University hospitals of Geneva, Geneva, Switzerland
2 Department of medicine, General Internal Medicine Service, University hospitals of Geneva, Geneva, Switzerland
Corresponding author: Dr Pierre Louge, Diving and hyperbaric Unit, University hospitals of Geneva, Geneva, Switzerland
Keywords
Blinding; Hyperbaric research; Placebo; Research methods
Abstract
(Louge P, Pignel R, Serratrice J, Stirnemann J. Validation of sham treatment in hyperbaric medicine: a randomised trial. Diving and Hyperbaric Medicine. 2023 March 31;53(1):51–54. doi: 10.28920/dhm53.1.51-54. PMID: 36966522. PMCID: PMC10318180.)
Introduction: This study aimed to determine the lowest possible atmospheric pressure in the 111−152 kPa (1.1−1.5 atmospheres absolute [atm abs]) range that would require the patients to equalise their ears, allowing an effective sham for a 203 kPa (2.0 atm abs) hyperbaric exposure.
Methods: We performed a randomised controlled study on 60 volunteers divided into 3 groups (compression to 111, 132 and 152 kPa (1.1, 1.3, 1.5 atm abs) to determine the minimum pressure to obtain blinding. Secondly, we applied confounding factors (faster compression with ventilation during the fictitious compression time, heating at compression, cooling at decompression) on 25 new volunteers in order to enhance blinding.
Results: The number of participants who did not believe they had been compressed to 203 kPa was significantly higher in the 111 kPa compressed arm than in the other two arms (11/18 vs 5/19 and 4/18 respectively; P = 0.049 and P = 0.041, Fisher’s exact test). There was no difference between compressions to 132 and 152 kPa. By applying additional confounding factors, the number of participants who believed they had been compressed to 203 kPa increased to 86.5 %.
Conclusions: A compression to 132 kPa, (1.3 atm abs, 3 metres of seawater equivalent) combined with the confounding elements of forced ventilation, enclosure heating and compression in five minutes, simulates a therapeutic compression table and can be used as a hyperbaric placebo.
Copyright: This article is the copyright of the authors who grant Diving and Hyperbaric Medicine a non-exclusive licence to publish the article in electronic and other forms.
Publication Type: Short communication
Full article available here.
- Super User
- Category: Information
- 11554
2023 June;53(2)
Diving Hyperb Med. 2023 June 30;53(2):76-84. doi: 10.28920/dhm53.1.76-84. PMID: 37365124. PMCID: PMC10584389.
Compressed gas diving fatalities in Australian waters 2014 to 2018
John Lippmann1,2,3, Christopher Lawrence4, Andrew Fock5
1 Australasian Diving Safety Foundation, Canterbury, Victoria, Australia
2 Department of Public Health and Preventive Medicine, Monash University, Victoria, Australia
3 Royal Life Saving Society Australia, Sydney, Australia
4 Statewide Forensic Medical Services, Royal Hobart Hospital, Tasmania, Australia
5 Department of Diving and Hyperbaric Medicine, The Alfred, Prahran, Victoria, Australia
Corresponding author: Dr John Lippmann, Australasian Diving Safety Foundation, PO Box 478, Canterbury, VIC 3126, Australia
Keywords
Carbon monoxide; Cardiovascular; Diving deaths; Fitness to dive; Obesity; Scuba
Abstract
(Lippmann J, Lawrence C, Fock A. Compressed gas diving fatalities in Australian waters, 2014 to 2018. Diving and Hyperbaric Medicine. 2023 June 30;53(2):76−84. doi: 10.28920/dhm53.2.76-84. PMID: 37365124. PMCID: PMC10584389.)
Introduction: This study aimed to investigate compressed gas diving deaths in Australia from 2014–2018 and make comparison to those from 2001–2013 to identify ongoing problems and assess countermeasures.
Methods: Media reports and the National Coronial Information System were searched to identify scuba diving deaths for 2014–2018, inclusive. Data were extracted from the witness and police reports, medical histories, and autopsies. An Excel® database was created and a chain of events analysis conducted. Comparisons were made with the earlier report.
Results: Forty-two fatalities were identified, 38 using scuba and four using surface-supplied breathing apparatus involving 30 males and 12 females. The mean age of victims was 49.7 years, six years higher than the previous cohort. Fifty-four percent were obese. Six victims were unqualified, three were under instruction and at least 28 were experienced divers, significantly more than in the previous cohort. Health-related predisposing factors, predominantly obesity and cardiac-related, were identified as likely contributory to 26 incidents, and planning shortcomings to at least 22 deaths. One-third of the disabling conditions were primary drowning and one-quarter were cardiac. Three divers died subsequent to carbon monoxide poisoning and three likely from immersion pulmonary oedema.
Conclusions: Advancing age, obesity and the associated cardiac disease have become increasingly prevalent in diving fatalities and the need for appropriate assessment of fitness to dive is evident.
Copyright: This article is the copyright of the authors who grant Diving and Hyperbaric Medicine a non-exclusive licence to publish the article in electronic and other forms.
Publication Type: Original article
Full article available here.
Diving Hyperb Med. 2023 June 30;53(2):85−91. doi: 10.28920/dhm53.2.85-91. PMID: 37365125. PMCID: PMC10586871.
Effectiveness of hyperbaric chamber ventilation
Lyubisa Matity1, Francois Burman2, Jacek Kot3, Joseph Caruana4
1 Hyperbaric and Tissue Viability Unit, Gozo General Hospital, Victoria VCT 2520, Malta
2 Divers Alert Network, Durham NC, USA
3 National Centre for Hyperbaric Medicine, Medical University of Gdańsk, Poland
4 Department of Physics, University of Malta, Msida MSD 2080, Malta
Corresponding author: Dr Lyubisa Matity, Hillside, Triq Gorg Mifsud Chircop, Qormi QRM 1591, Malta
Keywords
Carbon dioxide; Fire or explosion; Hyperbaric oxygen; Life support; Oxygen; Pressure
Abstract
(Matity L, Burman F, Kot J, Caruana J. Effectiveness of hyperbaric chamber ventilation. Diving and Hyperbaric Medicine. 2023 June 30;53(2):85−91. doi: 10.28920/dhm53.2.85-91. PMID: 37365125. PMCID: PMC10586871.)
Introduction: Hyperbaric chamber ventilation (HCV) refers to the intentional introduction of fresh gas, whether air, oxygen, or heliox, into a pressurised hyperbaric chamber in order to remove stale or otherwise compromised gas. The minimum required continuous HCV rate is usually determined by mathematical models derived from the contaminant mass balance within a well-stirred compartment. Non-uniform contaminant distribution patterns inside a hyperbaric chamber could emerge and invalidate the predictions of well-stirred models.
Methods: Contaminant distribution was investigated inside a clinical hyperbaric chamber with the aim of comparing well-stirred model predictions with the actual contaminant concentration measurements.
Results: Local ventilation effectiveness inside a clinical hyperbaric chamber may be compromised, leading to higher contaminant concentration values compared to the predictions of a mathematical model with a well-stirred assumption.
Conclusions: A well-stirred assumption in mathematical models is a useful simplification that allows reasonably accurate estimates of HCV requirements. However, local ventilation effectiveness values in a particular hyperbaric chamber might vary, with the potential for hazardous contaminant accumulation in under-ventilated zones.
Copyright: This article is the copyright of the authors who grant Diving and Hyperbaric Medicine a non-exclusive licence to publish the article in electronic and other forms.
Publication Type: Original article
Full article available here.
Diving Hyperb Med. 2023 June 30;53(2):92−99. doi: 10.28920/dhm53.2.92-99. PMID: 37365126. PMCID: PMC10586870.
Determining best practice for technical assessment of hookah surface supply diving equipment during diving fatality investigation
Darren Meehan1, David Smart1, John Lippmann2,3,4
1 Department of Diving and Hyperbaric Medicine, Royal Hobart Hospital, Hobart, Tasmania, Australia
2 Australasian Diving Safety Foundation, Victoria, Australia
3 Department of Public Health and Preventive Medicine, Monash University, Victoria, Australia
4 The Royal Lifesaving Society – Australia, Sydney, Australia
Corresponding author: Dr Darren Meehan, Department of Diving and Hyperbaric Medicine, Royal Hobart Hospital, 26 Campbell St, Hobart 7000, Tasmania, Australia
Keywords
Diving deaths; Investigations; Surface supply breathing apparatus; SSBA
Abstract
(Meehan D, Smart D, Lippmann J. Determining best practice for technical assessment of hookah surface supply diving equipment during diving fatality investigation. Diving and Hyperbaric Medicine. 2023 June 30;53(2):92−99. doi: 10.28920/dhm53.2.92-99. PMID: 37365126. PMCID: PMC10586870.)
Introduction: This study aimed to develop a standard process and checklist for technical investigation of hookah diving equipment and apply it to Tasmanian hookah fatality investigations from the last 25 years.
Methods: A literature search was undertaken to identify technical reports and equipment investigations associated with diving accidents. The information was assimilated to create a process and checklist for specifically assessing the hookah apparatus. The checklist was then applied in a gap analysis of Tasmanian hookah diving fatality technical reports from 1995 to 2019.
Results: As no papers specifically describing technical evaluation of hookah equipment were identified, references evaluating scuba equipment were used to create a hookah technical assessment process incorporating unique features of the hookah. Features included: owner responsibility for air quality; maintenance, function; exhaust proximity to air intake; reservoir volume; output non-return valves; line pressure; sufficiency of supply; entanglement; hose severance risk; gas supply failure and hosing attachment to the diver. Seven hookah diving deaths occurred in Tasmania (1995−2019) of which three had documented technical assessment. Gap analysis identified inconsistent structure between reports with variability in the case descriptors. Missing technical data included: overview of the hookah systems; accessories; weights; how the apparatus was worn by the diver; compressor suitability; assessment of hookah function; breathing gas output and exhaust position relative to air intake.
Conclusions: The study demonstrated a need to standardise technical reporting of hookah equipment after diving accidents. The checklist generated may serve as a resource for future hookah assessments and inform strategies for preventing future hookah accidents.
Copyright: This article is the copyright of the authors who grant Diving and Hyperbaric Medicine a non-exclusive licence to publish the article in electronic and other forms.
Publication Type: Original article
Full article available here.
Diving Hyperb Med. 2023 June 30;53(2):100−110. doi: 10.28920/dhm53.2.100-110. PMID: 37365127. PMCID: PMC10584396.
Technical validation of the EMMA capnometer under hyperbaric conditions
Alicia Tucker1, David Smart1
1 Department of Diving and Hyperbaric Medicine, Royal Hobart Hospital, Hobart, Tasmania, Australia
Corresponding author: Dr Alicia Tucker, Department of Diving and Hyperbaric Medicine, Royal Hobart Hospital, 26 Campbell St, Hobart 7000, Tasmania, Australia
ORCiD ID: 0000-0003-3578-8320
Keywords
Carbon dioxide; Capnography; Hyperbaric oxygen treatment; Intensive care medicine; Patient monitoring
Abstract
(Tucker A, Smart D. Technical validation of the EMMA capnometer under hyperbaric conditions. Diving and Hyperbaric Medicine. 2023 June 30;53(2):100−110. doi: 10.28920/dhm53.2.100-110. PMID: 37365127. PMCID: PMC10584396.)
Introduction: End-tidal carbon dioxide (ETCO2) monitoring is essential for monitoring intubated critical care patients, yet its use in hyperbaric environments can be problematic. We postulated that the EMMA mainstream capnometer may function accurately under hyperbaric conditions.
Methods: Stage 1. The EMMA mainstream capnometer was tested at 101 kPa against a reference side-stream capnometer, Philips IntelliVue M3015B microstream, using 10 customised reference gases of various carbon dioxide (CO2) concentrations (2.47%−8.09%, or 18.5−60.7 mmHg at 101 kPa) in either air or oxygen. Stage 2. The functionality and accuracy of the EMMA capnometer was tested under hyperbaric conditions, 121–281 kPa, using the same test gases.
Results: At 101 kPa, the EMMA capnometer measured CO2 at levels lower than expected (mean of differences = -2.5 mmHg (95% CI -2.1 to -2.9, P < 0.001)). The Philips capnometer measured CO2 more closely to expected CO2 (mean of differences = -1.1 mmHg (95% CI -0.69 to -1.4, P < 0.001). Both devices demonstrated a significant linear relationship with expected CO2. The EMMA capnometer functioned up to the maximum test pressure (281 kPa). The device over-read CO2 measurements at pressures > 141 kPa. Although variance increased at pressures in the therapeutic range for hyperbaric treatments, a significant linear relationship between expected and EMMA measured CO2 was demonstrated. The EMMA capnometer tolerated pressures to 281 kPa, but its display was limited to CO2 < 99 mmHg.
Conclusions: This study validated EMMA capnometer function to 281 kPa in the hyperbaric environment. The device over-read CO2 measurements at pressures >141 kPa, however there was a linear relationship between expected and measured CO2. The EMMA capnometer may be clinically useful for monitoring expired CO2 in patients undergoing hyperbaric oxygen treatment.
Copyright: This article is the copyright of the authors who grant Diving and Hyperbaric Medicine a non-exclusive licence to publish the article in electronic and other forms.
Publication Type: Original article
Full article available here.
Diving Hyperb Med. 2023 June 30;53(2):111−119. doi: 10.28920/dhm53.2.111-119. PMID: 37365128. PMCID: PMC10584393.
Hyperbaric oxygen and treadmill exercise partially prevented bone loss and bone microarchitecture deterioration in ovariectomized rats
Xiaoling Peng1, Binli Gao1, Xiangxiu Wang2, Xiaohong Qin3, Mei Peng1, Xianrong Zeng1
1 Department of Hyperbaric Oxygen, Sichuan Provincial People’s Hospital, University of Electronic Science and Technology of China, Chengdu, Sichuan Province, People’s Republic of China
2 Key Laboratory of Rehabilitation Medicine, West China Hospital, Sichuan University, Chengdu, Sichuan Province, People’s Republic of China
3 Sichuan Provincial Center for Mental Health, The Center of Psychosomatic Medicine of Sichuan Provincial People’s Hospital, University of Electronic Science and Technology of China, Chengdu, China
Corresponding author: Professor Xianrong Zeng, 32# W. Sec 2, 1st Ring Rd, Chengdu City, Sichuan Province, People’s Republic of China
Keywords
Animal model; Endocrinology; Hyperbaric oxygen treatment; Osteoporosis; Ovariectomy
Abstract
(Peng X, Gao B, Wang X, Qin X, Peng M, Zeng X. Hyperbaric oxygen and treadmill exercise partially prevented bone loss and bone microarchitecture deterioration in ovariectomized rats. Diving and Hyperbaric Medicine. 2023 June 30;53(2):111−119. doi: 10.28920/dhm53.2.111-119. PMID: 37365128. PMCID: PMC10584393.)
Introduction: Previous studies have demonstrated the beneficial effects of treadmill exercise (EX) on osteoporosis, and of hyperbaric oxygen (HBO) on osteoblast and osteoclast formation in vitro. We investigated the effects of HBO and the combination of HBO and EX on osteoporosis in ovariectomized rats.
Methods: Forty 3-month-old female Sprague-Dawley rats were randomly divided into 5 groups (n = 8): a sham control group (Control); an ovariectomy group; an ovariectomy with treadmill exercise treatment group; an ovariectomy with HBO treatment group; and an ovariectomy with HBO treatment combined with treadmill exercise group. The HBO exposures were 203 kPa, 85–90% O2, 90 min and the exercise regimen was 20 m·min-1, 40 min·day1, 5o slope. Both treatments were administered once daily, five days a week for 12 weeks until the rats were sacrificed.
Results: All three treatments (HBO, exercise, and both combined) significantly promoted the expression of the osteoblast‐related gene and oxidative metabolism-related gene (PGC-1α). They also exerted significant inhibitory effects on the osteoclast‐related mRNA expression (RANKL) and bone resorption marker CTX‐I. Additionally, exercise and the combination exercise-HBO treatment increased serum superoxide dysmutase (SOD) and sclerostin expression. No significant between-group difference was observed.
Conclusions: Hyperbaric oxygen, exercise, and the combination ameliorated bone microarchitecture deterioration and ovariectomy-induced bone loss in rats, and these inhibitory effects may be associated with the increased SOD and up-regulated PGC-1α.
Copyright: This article is the copyright of the authors who grant Diving and Hyperbaric Medicine a non-exclusive licence to publish the article in electronic and other forms.
Publication Type: Original article
Full article available here.
Diving Hyperb Med. 2023 June 30;53(2):120−128. doi: 10.28920/dhm53.2.120-128. PMID: 37365129. PMCID: PMC10584392.
How fit are military hyperbaric personnel after an asymptomatic or mild symptomatic COVID-19 infection? A retrospective study
Jan-Peter Schaap1, Margy E Zuluaga Fernandez2, Antoinette Houtkooper1, Edwin L Endert1, Pieter-Jan AM van Ooij1,3
1 Royal Netherlands Navy Diving and Submarine Medical Center, 1780 CA Den Helder, The Netherlands
2 Center for Man in Aviation, Royal Netherlands Air Force, 3769 DE Soesterberg, The Netherlands
3 Department of Pulmonary Medicine, Amsterdam University Medical Center, Amsterdam, The Netherlands
Corresponding author: Dr Pieter-Jan AM van Ooij, Royal Netherlands Navy Diving and Submarine Medical Center, 1780 CA Den Helder, The Netherlands
Keywords
Fitness to dive; Health status; Health surveillance; Infectious diseases; Lung; Lung function; Pulmonary function
Abstract
(Schaap J-P, Zuluaga Fernandez ME, Houtkooper A, Endert EL, van Ooij P-J AM. How fit are military hyperbaric personnel after an asymptomatic or mild symptomatic COVID-19 infection? A retrospective study. Diving and Hyperbaric Medicine. 2023 June 30;53(2):120−128. doi: 10.28920/dhm53.2.120-128. PMID: 37365129. PMCID: PMC10584392.)
Introduction: In the diving community there is a special need to know if asymptomatic or mild COVID-19 disease impacts the cardiopulmonary functioning of individuals with occupational exposure to extreme environments. To date, no controlled studies have been conducted comparing COVID-19-infected hyperbaric employees and non-COVID-19-infected peers in a military setting.
Methods: Between June 2020 and June 2021, healthy, hyperbaric, military personnel aged between 18 and 54 years old, who had recovered from asymptomatic or subclinical COVID-19 disease at least one month earlier, were analysed. Non-COVID-infected peers with medical assessments during the same period were used as the control group. Somatometry, spirometry, VO2 max, and DLCO were measured for each group.
Results: No clinically relevant differences in somatometry, lung function tests, and exercise testing were found between the COVID-19 group and the controls. However, the percentage of individuals with a decrease in estimated VO2-max of 10% or more was significantly greater in the COVID group than in the control group (24 vs. 7.8%, P = 0.004).
Conclusions: After asymptomatic or mild symptomatic COVID-19 infections, military hyperbaric employees are as fit as those who had not encountered COVID-19. As this research was based on a military population, it cannot be extrapolated to a nonmilitary population. Further studies in nonmilitary populations are necessary to determine the medical relevance of the present findings.
Copyright: This article is the copyright of the authors who grant Diving and Hyperbaric Medicine a non-exclusive licence to publish the article in electronic and other forms.
Publication Type: Original article
Full article available here.
Diving Hyperb Med. 2023 June 30;53(2):129−137. doi: 10.28920/dhm53.2.129-137. PMID: 37365130. PMCID: PMC10584397.
Evaluation of a new hyperbaric oxygen ventilator during volume-controlled ventilation
Cong Wang1, Lianbi Xue1, Qiuhong Yu1, Yaling Liu1, Ziqi Ren1, Ying Liu1
1 Department of Hyperbaric Oxygen, Beijing Tiantan Hospital, Capital Medical University, Beijing, China
Corresponding author: Dr Lianbi Xue, Department of Hyperbaric Oxygen, Beijing Tiantan Hospital, Capital Medical University, A zone, No.199, Nansihuan West Road, Fengtai District, Beijing (100070)
Keywords
Airway resistance; Intensive care; Intermittent positive-pressure ventilation; Respiratory mechanics
Abstract
(Wang C, Xue L, Yu Q, Liu Y, Ren Z, Liu Y. Evaluation of a new hyperbaric oxygen ventilator during volume-controlled ventilation. Diving and Hyperbaric Medicine. 2023 June 30;53(2):129−137. doi: 10.28920/dhm53.2.129-137. PMID: 37365130. PMCID: PMC10584397.)
Introduction: The performance of the Shangrila590 hyperbaric ventilator (Beijing Aeonmed Company, Beijing, China) was evaluated during volume-controlled ventilation.
Methods: Experiments were conducted in a multiplace hyperbaric chamber at 101, 152, 203, and 284 kPa (1.0, 1.5, 2.0 and 2.8 atmospheres absolute [atm abs]). With the ventilator in volume control ventilation (VCV) mode and connected to a test lung, comparison was made of the set tidal volume (VTset) versus delivered tidal volume (VT) and minute volume (MV) at VTset between 400 and 1,000 mL. Peak inspiratory pressure was also recorded. All measurements were made across 20 respiratory cycles.
Results: Across all ambient pressures and ventilator settings the difference between VTset and actual VT and between predicted MV and actual MV were small and clinically insignificant despite reaching statistical significance. Predictably, Ppeak increased at higher ambient pressures. With VTset 1,000 mL at 2.8 atm abs the ventilator produced significantly greater VT, MV and Ppeak.
Conclusions: This new ventilator designed for use in hyperbaric environments performs well. It provides relatively stable VT and MV during VCV with VTset from 400 mL to 800 mL at ambient pressures from 1.0 to 2.8 atm abs, as well as VTset 1,000 mL at ambient pressures from 1.0 to 2.0 atm abs.
Copyright: This article is the copyright of the authors who grant Diving and Hyperbaric Medicine a non-exclusive licence to publish the article in electronic and other forms.
Publication Type: Technical report
Full article available here.
Diving Hyperb Med. 2023 June 30;53(2):138−141. doi: 10.28920/dhm53.2.138-141. PMID: 37365131. PMCID: PMC10584399.
Hyperbaric medicine in Canadian undergraduate medical school curriculum
Zoé Talbot1, Alex Lee1, Sylvain Boet2-7
1 Faculty of Medicine, University of Ottawa, ON, Canada
2 Francophone Affairs, Faculty of Medicine, University of Ottawa, Ottawa, ON, Canada
3 Institut du Savoir Montfort, Ottawa, ON, Canada
4 Ottawa Hospital Research Institute, Clinical Epidemiology Program, Ottawa, ON, Canada
5 Department of Anesthesiology and Pain Medicine, The Ottawa Hospital, University of Ottawa, Ottawa, ON, Canada
6 Department of Innovation in Medical Education, University of Ottawa, Ottawa, ON, Canada
7 Faculty of Education, University of Ottawa, Ottawa, ON, Canada
Corresponding author: Dr Sylvain Boet, Department of Anesthesiology and Pain Medicine and Department of Innovation in Medical Education, The Ottawa Hospital, General Campus, 501 Smyth Rd, Critical Care Wing 1401, Ottawa, K1H 8L6, Ontario, Canada
Keywords
Education; Hyperbaric oxygen treatment; Teaching
Abstract
(Talbot Z, Lee A, Boet S. Hyperbaric medicine in Canadian undergraduate medical school curriculum. Diving and Hyperbaric Medicine. 2023 June 30;53(2):138−141. doi: 10.28920/dhm53.2.138-141. PMID: 37365131. PMCID: PMC10584399.)
Introduction: Hyperbaric oxygen treatment (HBOT) has fourteen approved indications in the management of acute and chronic diseases in various medical specialties. However, lack of physician knowledge and exposure to hyperbaric medicine may hinder the ability of patients to access this treatment option for approved indications. We aimed to determine the prevalence and nature of HBOT-related learning objectives in Canadian undergraduate medical education programs.
Methods: Pre-clerkship and clerkship learning objectives from responding Canadian medical schools’ curricula were reviewed. These were acquired through the school websites or by emailing the faculties. Descriptive statistics were used to summarise the number of hyperbaric medicine objectives taught in Canadian medical schools, and within each institution.
Results: Learning objectives from seven of the 17 Canadian medical schools were received and reviewed. From the curriculum of the responding schools, only one objective was found to be related to hyperbaric medicine. Hyperbaric medicine was absent from the other six schools’ objectives.
Conclusions: Based on the responding Canadian medical schools, hyperbaric medicine objectives were mostly absent from undergraduate medical curricula. These findings illustrate a possible gap in HBOT education and the need for discussion regarding the design and implementation of HBOT educational initiatives in medical training.
Copyright: This article is the copyright of the authors who grant Diving and Hyperbaric Medicine a non-exclusive licence to publish the article in electronic and other forms.
Publication Type: Short communication
Full article available here.
Diving Hyperb Med. 2023 June 30;53(2):142−146. doi: 10.28920/dhm53.2.142-146. PMID: 37365132. PMCID: PMC10584388.
Rebreather Forum Four consensus statements
Simon J Mitchell1,2,3, Neal W Pollock4,5
1 Department of Anaesthesiology, University of Auckland, Auckland, New Zealand
2 Department of Anaesthesia, Auckland City Hospital, Auckland, New Zealand
3 Slark Hyperbaric Unit, North Shore Hospital, Auckland, New Zealand
4 Department of Kinesiology, Université Laval, Québec, Canada
5 Service de médecine hyperbare, Centre de médecine de plongée du Québec, Hôtel-Dieu de Lévis, Québec, Canada
Corresponding author: Professor Simon J Mitchell, Department of Anaesthesiology, School of Medicine, University of Auckland, Private Bag 92019, Auckland 1142, New Zealand
Keywords
Accidents; Checklists; Decompression; Education; Equipment; Safety; Technical diving; Training
Abstract
(Mitchell SJ, Pollock NW. Rebreather Forum Four consensus statements. Diving and Hyperbaric Medicine. 2023 June 30;53(2):142−146. doi: 10.28920/dhm53.2.142-146. PMID: 37365132. PMCID: PMC10584388.)
Closed circuit rebreathers have been widely adopted by technical divers as tools for reducing gas consumption and extending depth and duration capabilities. Rebreathers are technologically complex with many failure points, and their use appears associated with a higher accident rate than open circuit scuba. Rebreather Forum Four (RF4) was held in Malta in April 2023 attracting approximately 300 attendees and representatives of multiple manufacturers and training agencies. Over two and a half days a series of lectures was given by influential divers, engineers, researchers and educators on topics of contemporary relevance to rebreather diving safety. Each lecture was followed by a discussion session with audience participation. Potential consensus statements were drafted by the authors (SJM and NWP) during the course of the meeting. These were worded to be confluent with some important messages emerging from the presentations and subsequent discussions. The statements were presented one by one in a half-day plenary session of participants, and discussion was invited on each. After discussion and any necessary revision, the participants voted on whether to adopt the statement as a position of the forum. A clear majority was required for acceptance. Twenty-eight statements embracing thematic areas designated ‘safety’, ‘research’, ‘operational issues’, ‘education and training’, and ‘engineering’ were adopted. Those statements are presented along with contextualising narrative where necessary. The statements may help shape research and teaching initiatives, and research and development strategies over subsequent years.
Copyright: This article is the copyright of the authors who grant Diving and Hyperbaric Medicine a non-exclusive licence to publish the article in electronic and other forms.
Publication Type: Short communication
Full article available here.
Diving Hyperb Med. 2023 June 30;53(2):147−150. doi: 10.28920/dhm53.2.147-150. PMID: 37365133. PMCID: PMC10584400.
Successful hyperbaric oxygen treatment of a patient with a HeartMate III left ventricular assist device
Arun Ilancheran1,2, Ian Millar1,2, Theo Tsouras1
1 Hyperbaric Service, Alfred Health, Melbourne, Australia
2 Monash University, Melbourne, Australia
Corresponding author: Dr Arun Ilancheran, Hyperbaric Unit, Main Ward Block, Level 1, 55 Commercial Rd, Melbourne VIC 3004, Australia
ORCiD: 0000-0002-3341-8134
Keywords
Bioengineering; Case report; LVAD; Haemorrhagic cystitis
Abstract
(Ilancheran A, Millar I, Tsouras T. Successful hyperbaric oxygen treatment of a patient with a HeartMate III left ventricular assist device. Diving and Hyperbaric Medicine. 2023 June 30;53(2):147−150. doi: 10.28920/dhm53.2.147-150. PMID: 37365133. PMCID: PMC10584400.)
A 53-year-old woman with a HeartMate III left ventricular assist device (LVAD) was successfully treated under hyperbaric conditions for haemorrhagic cystitis. The HeartMate III LVAD inserted in this patient had not previously been tested or certified for use under hyperbaric conditions. To our knowledge this is the first report of the HeartMate III LVAD being used to support a patient undergoing hyperbaric treatment. The overview detailed here of the safety and technical aspects of managing this patient for hyperbaric treatment was possible due to the collaboration of a multi-disciplinary team. We believe that our experience has demonstrated a pathway to safe hyperbaric treatment of patients dependent upon a HeartMate III LVAD.
Copyright: This article is the copyright of the authors who grant Diving and Hyperbaric Medicine a non-exclusive licence to publish the article in electronic and other forms.
Publication Type: Case report
Full article available here.
Diving Hyperb Med. 2023 June 30;53(2):151−154. doi: 10.28920/dhm53.2.151-154. PMID: 37365134. PMCID: PMC10584398.
Successful delayed treatment of acute glans penis ischaemia after adult circumcision: a case report
Kenneth Lo1,2, Darren Katz3,4,5, Vincent Chan3,5, Ian Millar1
1 Department of Intensive Care and Hyperbaric Medicine, Alfred Health, Melbourne, Australia
2 Department of Emergency Medicine, Alfred Health, Melbourne, Australia
3 Men’s Health Melbourne, Victoria, Australia
4 Department of Surgery, Western Precinct, University of Melbourne, Victoria, Australia
5 Department of Urology, Western Health, Victoria, Australia
Corresponding author: Dr Kenneth Lo, Hyperbaric Unit, Main Ward Block, Level 1, 55 Commercial Rd, Melbourne VIC 3004, Australia
Keywords
Anticoagulation; Case report; Hyperbaric oxygen; Surgery; Tadalafil
Abstract
(Lo K, Katz D, Chan V, Millar I. Successful delayed treatment of acute glans penis ischaemia after adult circumcision: a case report. Diving and Hyperbaric Medicine. 2023 June 30;53(2):151−154. doi: 10.28920/dhm53.2.151-154. PMID: 37365134. PMCID: PMC10584398.)
Penile glans ischaemia post-circumcision is very rare. A 20-year-old male presented with glans ischaemia following an elective circumcision and was successfully treated with a combination of subcutaneous injection of low molecular weight heparin 0.5 mg·kg-1 twice-daily, oral Tadalafil 5 mg once-daily for three days and 12 hyperbaric oxygen treatments at 243 kPa (2.4 atmospheres absolute) beginning 48 hours after the onset of ischaemia.
Copyright: This article is the copyright of the authors who grant Diving and Hyperbaric Medicine a non-exclusive licence to publish the article in electronic and other forms.
Publication Type: Case report
Full article available here.
Diving Hyperb Med. 2023 June 30;53(2):155−157. doi: 10.28920/dhm53.2.155-157. PMID: 37365135. PMCID: PMC10584395.
Hemiplegia resulting from acute carbon monoxide poisoning
Burak Turgut1, Kübra Canarslan Demir1, Gözde Büşra Sarıyerli Dursun1, Taylan Zaman1
1 Department of Underwater and Hyperbaric Medicine, University of Health Sciences, Gulhane Training and Research Hospital, Ankara, Turkey
Corresponding author: Dr Burak Turgut, SBÜ-Gülhane Eğitim ve Araştırma Hastanesi, Sualtı Hekimliği ve Hiperbarik Tıp Kliniği, Etlik/Ankara, Turkey
ORCiD: 0000-0002-9638-6221
Keywords
Case reports; Hyperbaric oxygen treatment; Neurological manifestations; Recovery of function
Abstract
(Turgut B, Canarslan Demir K, Sarıyerli Dursun GB, Zaman T. Hemiplegia resulting from acute carbon monoxide poisoning. Diving and Hyperbaric Medicine. 2023 June 30;53(2):155−157. doi: 10.28920/dhm53.2.155-157. PMID: 37365135. PMCID: PMC10584395.)
Carbon monoxide (CO) poisoning can cause neurological complications such as movement disorders and cognitive impairment through hypoxic brain damage. Although peripheral neuropathy of the lower extremities is a known complication of CO poisoning, hemiplegia is very rare. In our case, a patient who developed left hemiplegia due to acute CO poisoning received early hyperbaric oxygen treatment (HBOT). The patient had left hemiplegia and anisocoria at the beginning of HBOT. Her Glasgow coma score was 8. A total of five sessions of HBOT at 243.2 kPa for 120 minutes were provided. At the end of the 5th session, the patient’s hemiplegia and anisocoria were completely resolved. Her Glasgow coma score was 15. After nine months of follow-up, she continues to live independently with no sequelae, including delayed neurological sequelae. Clinicians should be aware that CO poisoning can (rarely) present with hemiplegia.
Copyright: This article is the copyright of the authors who grant Diving and Hyperbaric Medicine a non-exclusive licence to publish the article in electronic and other forms.
Publication Type: Case report
Full article available here.
- Super User
- Category: Information
- 86
Diving and Hyperbaric Medicine Downloadable Digital Products Terms and Conditions of Sale
1.0 Introduction: These terms and conditions set out the terms and conditions between you, the customer, and Diving and Hyperbaric Medicine (“us”, “we”), governing the use of our website and our downloadable digital products including the content therein (the “products”). Your use of our website, and purchase, download and use of our products, constitutes your full acceptance of these terms and conditions. If you do not agree with these terms and conditions, you should not use our website or purchase, download or use any of our products.
2.0 License and Use: Your purchase of one of our products constitutes our granting to you of a non-exclusive, non-sublicensable, non-transferable license to download and access that product for the purpose of your own personal use and reference, and print or convert the product to an image or vector format for your own storage, retention and reference (the “purpose”). You agree that under no circumstances shall you use, or permit to be used, any product other than for the aforesaid purpose. For the avoidance of doubt, you shall not copy, re-sell, sublicense, rent out, share or otherwise distribute any of our products, whether modified or not, to any third party. You agree not to use any of our products in a way which might be detrimental to us or damage our reputation.
3.0 Intellectual Property: The products, whether modified or not, and all intellectual property and copyright contained therein, are and shall at all times remain our sole and exclusive property. You agree that under no circumstances, whether the product has been modified or not, shall you have or attempt to claim ownership of any intellectual property rights or copyright in the product.
4.0 Refunds and Chargebacks: Once a product has been purchased by you, no right of cancellation or refund exists under the Consumer Protection (Distance Selling) Regulations 2000 due to the electronic nature of our products. Any refunds shall be at our sole and absolute discretion. You agree that under no circumstances whatsoever shall you initiate any chargebacks via your payment provider. You agree that any payments made by you for any of our products are final and may not be charged back. We reserve the right to alter any of our prices from time to time.
5.0 Warranties and Liability: We make every effort to ensure that our products are accurate, authoritative and fit for the use of our customers. However, we take no responsibility whatsoever for the suitability of the product, and we provide no warranties as to the function or use of the product, whether express, implied or statutory, including without limitation any warranties of merchantability or fitness for particular purpose. You agree to indemnify us against all liabilities, claims, demands, expenses, actions, costs, damages, or loss arising out of your breach of these terms and conditions. Furthermore, we shall not be liable to you or any party for consequential, indirect, special or exemplary damages including but not limited to damages for loss of profits, business or anticipated benefits whether arising under tort, contract, negligence or otherwise whether or not foreseen, reasonably foreseeable or advised of the possibility of such damages.
6.0 General: These terms and conditions constitute the entire agreement and understanding between you and us for the supply of downloadable digital products, and shall supersede any prior agreements whether made in writing, orally, implied or otherwise. The failure by us to exercise or enforce any right(s) under these terms and conditions shall not be deemed to be a waiver of any such right(s) or operate so as to bar the exercise or enforcement thereof at any time(s) thereafter, as a waiver of another or constitute a continuing waiver. You agree that monetary damages may not be a sufficient remedy for the damage which may accrue to us by reason of your breach of these terms and conditions, therefore we shall be entitled to seek injunctive relief to enforce the obligations contained herein. The unenforceability of any single provision within these terms and conditions shall not affect any other provision hereof. These terms and conditions, your acceptance thereof, and our relationship with you shall be governed by and construed in accordance with English law and both us and you irrevocably submit to the exclusive jurisdiction of the English courts over any claim, dispute or matter arising under or in connection with these terms and conditions or our relationship with you.
Contacting Us: Please do not hesitate to contact us regarding any matter relating to this Diving and Hyperbaric Medicine Downloadable Digital Products Terms and Conditions of Sale Policy via email
- Super User
- Category: Information
- 6206
SPUMS on behalf of Diving and Hyperbaric Medicine Journal
Who are we?
SPUMS is the leading medical society representing doctors in the field of Diving and Hyperbaric Medicine in the South Pacific region.
Full membership is open to registered medical practitioners with an interest in Diving and/or Hyperbaric Medicine. Associate membership is also open to other health-care workers, medical students, educational organisations, commercial companies in the diving and hyperbaric fields and non-medical persons. Associate members do not have voting rights.
SPUMS is a not for profit medical society with the following purposes and aims:
- To promote and facilitate the study of all aspects of underwater and hyperbaric medicine.
- To provide information on underwater and hyperbaric medicine.
- To promote communication between members of the Association and to publish a journal for the Association.
- To convene members of the Association annually at a scientific conference and to hold meetings and other functions or activities to inform, and to develop fellowship and friendship amongst members of the Association.
A full copy of the Purposes and Rules is available on the SPUMS website: Privacy Policy
Our privacy commitment to you:
Confidentiality and privacy protection is essential for health care. SPUMS is not a healthcare provider. SPUMS facilitates the exchange and sharing of scientific information between members, and provides scientific information about underwater and hyperbaric medicine, and promotes best practice in the field.
We are committed to protecting the privacy and confidentiality of the information we collect from members, visitors to our website, people who contact us and from our suppliers and affiliates.
SPUMS is also required to comply with applicable Commonwealth, State and Territory privacy law. Under these privacy laws, we are required to comply with a set of privacy principles. The core principles are in the Privacy Act 1988. More information about these principles and Australian privacy law can be found on the Australian Information Commissioner’s website: www.oaic.gov.au
What information do we collect and store?
SPUMS collects personal information from members, persons enquiring or applying for membership, persons forwarding inquiries to executive committee members, and from our suppliers.
Information is mainly collected directly from the person concerned, including through emails, telephone calls, SPUMS website and mobile devices. We also collect this information from publicly available websites, directories and maps and via Facebook and other social media.
Many SPUMS medical members who have training in diving and hyperbaric medicine choose to have their name published on the SPUMS website as part of a register of doctors who perform dive medical assessments – Diving Doctors List (DDL). Members who are on the register must consent and supply the contact information that is published.
Why do we collect this information and what do we use it for?
SPUMS collects, stores and uses the information to provide services to our members, so that members can receive the scientific journal Diving and Hyperbaric Medicine (DHM), communications and updates of medical knowledge; to communicate society activities and events including the annual scientific meeting and other educational activities.
SPUMS publishes contact information about members who choose to be included on the DDL. This information is the doctor’s name, practice address and contact details. It also includes whether or not they undertake recreational or commercial medicals and paediatric diving medical assessments. This information is required so that a member of the public can contact the member at their practice to book an appointment.
We only provide others with information that would identify you if it is necessary to provide you with the service or information that you requested, you have agreed to us providing it to them or it is already publicly available information.
We provide your information to the DHM office which is based in New Zealand, and the mailing house for DHM, to permit mailing of the journal to your preferred address, or for email communications. SPUMS does not provide your personal information to any marketing companies, or other third parties, unless permission is granted by you.
You are entitled to see what information we hold about you:
Under Australian privacy law, you have rights of access to personal information that we hold about you. These rights also include correction of any errors in this information. SPUMS members are able to access and update their own personal information that is stored on the website, including practice details. If members have any concerns or queries regarding their personal information, they should contact the SPUMS Secretary: <
For how long do you keep my personal information?
Your personal information is kept active for as long as your membership is active, as is reasonably required to meet your needs. SPUMS is required to maintain a registry of members under Victorian state consumer law for reporting membership numbers (deidentified) each year.
We keep membership records and other personal information on file to enable us to undertake statistical and historical analysis and reporting. Unless otherwise requested, member’s details will be destroyed within two years of membership ceasing.
How is your information stored and protected?
Information is stored in electronic systems under our control and website information with contracted data storage providers. These providers may be located outside Australia and includes Cloud storage. We take appropriate steps to protect the security of the information we hold about you, including protections against unauthorised access, virus or other electronic intrusions, fire, theft or loss. Data is regularly backed up to maintain security.
SPUMS executive and support staff are bound by strict requirements regarding confidentiality and protection of the privacy of the information we collect and hold about you.
How do I obtain more information or have a complaint about SPUMS about privacy protection?
Please contact the